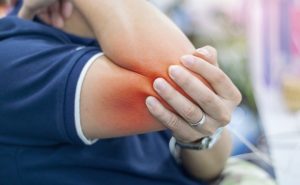
 Elbow pain is a common complaint among athletes, active individuals, and people who perform repetitive arm movements at work. Two of the most frequent causes are tennis elbow and golfer’s elbow. While their names suggest sports-related injuries, these conditions can affect anyone. Understanding the symptoms and treatment options helps patients recover effectively and prevent long-term issues. At the practice of Steven C. Thomas, MD and Donald W Pennington, DO, our board-certified surgeons specialize in orthopedic procedures in the Las Vegas area.
Elbow pain is a common complaint among athletes, active individuals, and people who perform repetitive arm movements at work. Two of the most frequent causes are tennis elbow and golfer’s elbow. While their names suggest sports-related injuries, these conditions can affect anyone. Understanding the symptoms and treatment options helps patients recover effectively and prevent long-term issues. At the practice of Steven C. Thomas, MD and Donald W Pennington, DO, our board-certified surgeons specialize in orthopedic procedures in the Las Vegas area.
What Is Tennis Elbow
Tennis elbow occurs when the tendons on the outside of the elbow become inflamed or damaged due to repetitive wrist and arm motions. It commonly affects people who perform gripping, lifting, or twisting movements, such as office workers, mechanics, and fitness enthusiasts.
What Is Golfer’s Elbow
Golfer’s elbow affects the tendons on the inside of the elbow. It is caused by repetitive wrist flexion or gripping motions. This condition is common among golfers, weightlifters, and individuals whose jobs involve repetitive hand use.
Common Symptoms of Elbow Tendon Injuries
Symptoms of both conditions may include pain, tenderness, and stiffness around the elbow. Pain may worsen with gripping, lifting objects, or rotating the forearm. Weakness in the hand or wrist is also common.
While tennis elbow causes pain on the outer elbow, golfer’s elbow causes pain on the inner side.
Non-Surgical Treatment Options
Most cases of tennis and golfer’s elbow improve with conservative care. Treatment options often include rest, activity modification, physical therapy, bracing, and anti-inflammatory medications. Physical therapy focuses on strengthening and stretching the forearm muscles to reduce strain on the tendons.
In some cases, injections or advanced therapies may be recommended to promote healing.
When Surgery Is Considered
Surgery is rarely needed but may be considered if symptoms persist despite several months of conservative treatment. Surgical procedures focus on removing damaged tissue and restoring tendon function.
Preventing Recurrence
Proper technique during activities, ergonomic adjustments, and strengthening exercises help prevent future flare-ups. Early treatment is key to avoiding chronic pain and prolonged recovery.
Contact Surgeons Dr. Thomas and Dr. Pennington at the Knee and Shoulder Institute in Las Vegas, NV to Schedule an Appointment:
If you would like to schedule an appointment or learn more about the Knee and Shoulder Institute procedures & treatments,contact the office today click here.
Serving patients from and around greater Las Vegas, Lake Havasu, Bullhead City, Mesquite, Pahrump, Nevada



 An ACL tear is one of the most common and significant knee injuries, especially among athletes and active individuals. The
An ACL tear is one of the most common and significant knee injuries, especially among athletes and active individuals. The  An
An  Arthroscopy is one of the most common orthopedic procedures performed today. This minimally invasive technique allows surgeons to see inside a joint using a small camera and specialized instruments, making it possible to diagnose and treat many conditions with less trauma than open surgery. But while
Arthroscopy is one of the most common orthopedic procedures performed today. This minimally invasive technique allows surgeons to see inside a joint using a small camera and specialized instruments, making it possible to diagnose and treat many conditions with less trauma than open surgery. But while 
 If
If